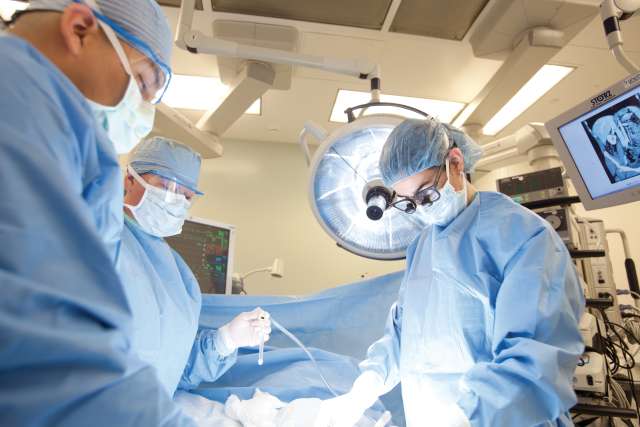
Endoscopic otologic surgery at UCLA Health offers patients with ear disease or injury an opportunity to achieve greater hearing health with a less invasive curative method as compared to more traditional approaches.
The new approach “is an important step forward,” says Andrew McCall, MD, associate professor of head and neck surgery at the David Geffen School of Medicine at UCLA.
Dr. McCall has been perfecting his skills with endoscopic otologic surgery over the past decade. He successfully performed UCLA’s first endoscopic tympanic membrane (eardrum) perforation repair at Ronald Reagan UCLA Medical Center. A leader in the use of surgical endoscopes in the ear, he teaches and mentors other surgeons in the advanced technique.
“Endoscopes allow for incredible visualization. What you can see with an endoscope is truly remarkable,” Dr. McCall says.
While he says endoscopes are not a replacement for traditional microscopes, which remain necessary in some ear surgeries, there are a variety of conditions for which the endoscopic approach may be superior.
“When we work with microscopes outside the body, beams of light travel in a straight line down the cylindrical ear canal to the area of interest. That only gives us a direct view of what is in our line of sight. We cannot see around the walls of the ear canal,” Dr. McCall explains. “That's where an endoscope has substantial advantages.
“We can put an angled endoscope camera down into the ear canal and see areas we could not see before. And by coupling an endoscope with some specialized instrumentation with curves on the end, we can reach around those corners and clear disease that previously would require additional procedures.”
‘Like a dance’
An otologic endoscope with a camera on its tip typically measures a slender 3 mm in width — larger than a pencil point and smaller than an eraser tip. During outpatient surgery, an endoscope is inserted into the ear canal of a patient under general anesthesia.
“General anesthesia is important as we’re working in very tight spaces with cramped anatomy,” says Dr. McCall. “The last thing we want somebody in the middle of that to do is move.”
The surgeon holds and guides the endoscope in one hand and manipulates the surgical instrumentation in the other hand. The careful maneuvering “takes coordination,” Dr. McCall says. “It’s almost like a dance.”
Endoscopes prove extremely helpful when dealing with problems with the eardrum or the middle ear, the area underneath the eardrum where the bones of the ear are located. Injury to these bones can cause conductive hearing loss.
“We can go through the ear canal, take out a problematic bone and put a prosthesis in its place — a tiny metal piece to reconnect the eardrum to the inner ear. That can be used to help restore hearing.”
Additionally, endoscopic surgery has been very successful in treating cholesteatoma, a destructive skin cyst that grows in the ear. The enhanced visualization afforded by the endoscope can allow surgeons a better opportunity to identify and clear disease, Dr. McCall notes.
Moreover, by being able to work around the corner of the ear canal with the endoscope, postauricular incisions can be avoided in many cases. The ability to avoid external incisions is one of the significant benefits endoscopic surgeries afford patients.
“Because they are less invasive, there is less post-operative pain and discomfort,” he says. “And of course, there is no visible scar.”
Who is a candidate?
Most patients, from pediatric to geriatric, are candidates for endoscopic otologic surgery if their condition warrants it.
“The decision to perform endoscopic ear surgery is more driven by disease or disease location than by patient mitigating factors,” says Dr. McCall. “If a patient can tolerate general anesthesia for microscopic ear surgery, I would expect them to tolerate it for endoscopic ear surgery as well.
“I would encourage physicians to refer patients with the conditions discussed earlier for evaluation to see if this more minimally invasive approach could be used.”
Once the decision is made to do endoscopic surgery, Dr. McCall says, a patient is advised that in the event a surgeon discovers the disease state requires more traditional surgery, it will be done at the same time – in one fell swoop.
“We always have a plan B, because we would not want a patient to have to unnecessarily return for a second procedure,” says Dr. McCall. “If we go in thinking we’re doing it endoscopically, there’s a very low chance of conversion to a microscopic surgery approach. Most of the time, we’re able to do it all through the ear canal.”