Mission Pillars
Find your care
If you’re admitted to the hospital, your primary care physician will ensure that you receive care from a UCLA Health hospitalist. Please call us at 855-488-9550 if you have questions.
Clinical Care
Procedures
Our UCLA Health hospitalists have strong in-hospital procedural support from our interventional radiology colleagues and a robust proceduralist service staffed by our hospitalists. The Procedure Service was started in 2015 as a part of the Hospitalist department in conjunction with the internal medicine residency program. It is staffed by a select group of hospitalists, dubbed "proceduralists," who have demonstrated an aptitude for procedures and teaching. The team is available for bedside ultrasound-guided procedures, including paracenteses, lumbar punctures, central venous catheter placement, and ultrasound-guided peripheral IVs. Hospitalists who are interested in joining the team receive extensive mentorship from senior proceduralists and complete procedure simulations in the simulation center. Once they demonstrate competency in performing procedures, they may become core members of the team with procedure service weeks integrated into their hospitalist schedule. Our proceduralists are also core educators who work closely with residents on the service and teach them best practices to help them build confidence in their bedside procedural skills. They also often help teach procedural skills in the medical school curriculum.
Medical Education
Medical Education
The UCLA Health hospital's Medicine has a strong commitment to educating future generations of physicians. Our faculty play key roles in nearly every aspect of medical education at the UCLA David Geffen School of Medicine and the UCLA Internal Medicine Residency, as well as in many initiatives beyond these institutions. Hospitalists participate in preclinical medical school activities, such as small group learning, simulation, and lectures at the David Geffen School of Medicine. Some of our hospitalists regularly work with pre-clinical medical students as Educators for Excellence, meeting weekly with a group of students to teach the basics of clinical medicine. Others are part of the Longitudinal Clinical Experience course, in which a 3rd-year medical student in their “Discovery” year is paired with faculty members to meet regularly in the clinical space. Others run individual simulations or other educational sessions. Our hospitalists also work closely with 4th-year medical students on a variety of clinical rotations, ranging from classic sub-internships to an innovative Advanced Hospitalist elective in which a 4th-year medical student works 1:1 with a direct-care hospitalist.
Our hospitalist faculty are also very engaged in medical education within the UCLA Internal Medicine Residency Program and other residency programs in the Los Angeles area. UCLA Health hospitalists rotate on teaching services across multiple UCLA Health institutions, as well as other community institutions, and are an integral part of the clinical educational experience for trainees. Beyond teaching clinical services, our faculty are involved in a broad spectrum of residency medical education. They often lead noon conference, morning reports, UCLA Department of Medicine Grand Rounds, and other didactic curricula. They have started innovative ultrasound and procedural electives. They are leaders of inclusive excellence, informatics, global health, evidence-based medicine, and many other curricula. Our hospitalists have received many teaching awards for their work in these areas, and the department prides itself on supporting its faculty in their educational roles, enabling growth and innovation.
Point of Care Ultrasound (POCUS)
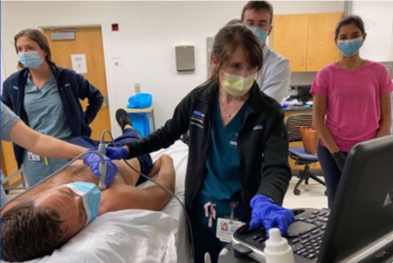
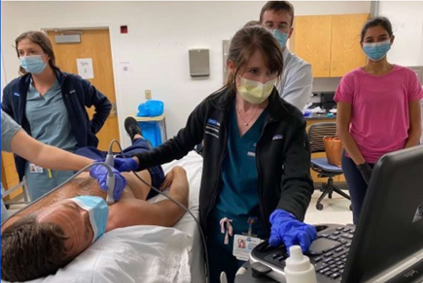
The UCLA Health Hospital Medicine is committed to advancing the use of Point-of-Care Ultrasound (POCUS) in clinical practice and to teaching POCUS to the next generation of physicians. Our hospitalists faculty have the opportunity to build their POCUS skills through a variety of educational sessions organized by Drs. Daniel Kahn and Reece Doughty, the Director and Associate Director of Bedside Ultrasound Education. These range from online modules to hands-on didactics to longitudinal image review and feedback. For those interested in teaching POCUS, there are multiple opportunities to teach internal medicine residents and medical students throughout the year.
Furthermore, we can upload POCUS images and videos to our electronic medical system to enhance patient care. We also maintain a UCLA POCUS website with extensive UCLA-specific and external ultrasound resources, a monthly ultrasound case series, and a journal club. Each year, we work to expand POCUS training and opportunities so that UCLA Health can remain a leader among academic institutions.

Simulation
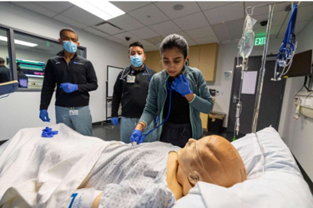
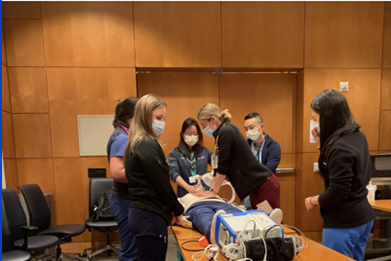
It has been well-established that simulation is an effective educational tool for undergraduate and graduate medical training. As such, our hospitalist section is highly engaged in teaching through simulation in a variety of different settings. First, the David Geffen School of Medicine and the UCLA Internal Medicine Residency Program each have a robust curriculum of simulation training at the recently renovated, state-of-the-art Rosenfeld Hall simulation center. Students and trainees participate regularly in half-day sessions using high-fidelity mannequin simulators. These are regularly led by hospitalist faculty, with ample opportunities throughout the year.
Additionally, our faculty are involved in curriculum design and the design of individual simulation cases. In addition to sessions held in the Rosenfeld Hall simulation center, a group of our UCLA Health hospitalists leads an innovative new simulation program called "in-situ simulations," through which residents at the UCLA Ronald Reagan Medical Center participate in short simulation cases in the hospital while on service. Virtual Reality simulation and other innovative simulation techniques are also being actively investigated by our faculty.

Research, Innovation & Scholarship
Several UCLA Health hospitalists are involved in research and scholarship, including in-clinical practices, medical education, quality improvement, bioinformatics, social medicine, value-based care, and health services research. In alignment with the UCLA Department of Medicine's strategic plan, we seek to increase the impact and profile of hospital medicine research both locally and nationally.
UCLA Health offers many services to researchers through the UCLA Clinical and Translational Science Institute, including consulting in study design, datasets, and statistical analysis.
Publications by UCLA Hospital Medicine
Research Spotlight
Dr. Russ Kerbel's work on artificial intelligence models in early detection of sepsis was featured in the February 2025 departmental newsletter.
Dr. Rich Leuchter's work on the Next Day Clinic was a Top Research Presentation at the SMH Converge 2025.

Quality Improvement
The goal of the UCLA Health Hospital Medicine Quality Improvement (QI) Program is to engage hospitalists in quality improvement through data sharing, collaboration, training, and mentorship to enhance the quality and delivery of care in our hospitals. In keeping with the spirit of the UCLA Department of Medicine's core values, our work focuses on improving patient outcomes, educating future quality-improvement leaders, and developing innovative solutions to system issues.
The section of hospital medicine has active initiatives in all areas of UCLA Health's MOVERS quality strategy: Morality, Outcomes, Value, Experience, Readmissions, and Safety. UCLA Health hospitalists also lead and participate in QI projects and committees through the department, hospital, and faculty practice group. Formal Lean training is offered to all interested hospitalists in collaboration with UCLA Performance Excellence.
Inclusive Excellence & Community Engagement
Commitment to Inclusive Excellence and Community Engagement
UCLA Health Medicine is committed to the principles of community engagement and inclusive excellence. Over the past several years, we have made great strides in fostering tangible improvements in these domains. We have restructured our hiring and recruitment committee to provide more equitable and holistic evaluations while improving the representation of equally qualified faculty from diverse backgrounds and life experiences. We actively teach residents, students, and hospitalists about implicit bias on our wards. We are rolling out a longitudinal professional development curriculum to improve our hospitalists' knowledge and comfort with these topics as they relate to healthcare and medical education.
The hospitalist medicine section is actively working to increase our engagement with the community. Our hospitalists work with the UCLA Homeless Healthcare Collaborative, a mobile outreach unit focused on caring for people experiencing homelessness, where they meet patients in the streets, in encampments, or in shelters to deliver medical care and social services to those most in need. They can provide post-discharge follow up care for the unhoused population, facilitate improved medication adherence, and coordinate primary and specialty care.
Additionally, we have several individual hospitalists engaged in mentorship activities at the high school, undergraduate and medical school levels. The UCLA Summer Health Professions Education Program and the UCLA Premedical Enrichment Programs are both pipeline programs intended to improve access and matriculation of underrepresented minorities into top-tier medical schools, and hospitalists can provide invaluable mentorship for these students.
Dr. Veronica Ramiez, the clinical lead of our Downtown cohort, is actively supporting multiple learners and faculty of Hispanic descent through her involvement in groups such as "First-Gen", a UCLA undergraduate student group for first-generation Hispanics, and the Latino Medical Student Association (LMSA), with the goal of increasing representation of these historically underrepresented groups in medicine.
Other opportunities for community involvement include participating in health fairs such as Care Harbor, which provides free medical, dental, and vision care to the uninsured, underinsured, and underserved in our communities. Some UCLA Hospitalist cohorts provide clinical care at MLKCH and Olive View-UCLA Medical Center, both of which are local safety net hospitals.
We understand that the health of our patients and the caliber of our medical education depend on optimizing community engagement and inclusive excellence in our clinical and teaching spaces, and we are committed to continuing to develop and foster this culture within UCLA Health Hospital Medicine.
Global Health
Several of our hospitalists are active in global health education in our medicine residency program and at the David Geffen School of Medicine at UCLA. In the Internal Medicine Global Health Pathway, they mentor, train, and supervise medical students and residents during their clinical engagements at partner sites in Malawi, Peru, Thailand, and Shiprock, New Mexico. They contribute to a longitudinal global health curriculum for medical residents, instructing on clinical and non-clinical topics such as ethics, decolonization, and global health equity. They utilize their hospital medicine skills in their practice and instruction abroad and apply their expertise in areas such as POCS to patients in low-resource settings.

